Caring for a loved one with a disability or a chronic condition is a journey filled with immense emotional and financial hurdles. For many Texas families, Texas Medicaid waiver programs are nothing short of a lifeline, opening the door to critical Medicaid-funded services right in your loved one's home instead of a nursing facility. We understand how overwhelming this process can feel, and our goal is to guide your family through it with clarity and care.
Think of a waiver as a special key. It unlocks a more personalized, compassionate path to care—one that champions independence and dignity by bringing support services into the community.
A Lifeline for Texas Families

When long-term care becomes a necessity, the options can feel distressingly institutional. Many Texas families assume a nursing home is the only viable path, a choice that’s as emotionally taxing as it is financially draining. Medicaid waiver programs present a powerful, practical alternative to that assumption.
These programs are specifically designed to provide home and community-based services (HCBS) to people who would otherwise need care in an institutional setting, like a nursing home or a state-supported living center. The term "waiver" is used because the federal government essentially "waives" certain Medicaid rules, giving states like Texas the flexibility to offer unique supports tailored to specific needs.
Understanding the Purpose of Waivers
At their core, these programs are about empowering people to live as independently as possible in their own communities. This approach doesn't just improve quality of life; it honors the profound value of familiar surroundings and the comfort of family support.
For families navigating a potential Guardianship, getting a firm grasp on these programs is absolutely essential. They are one of the primary tools for ensuring your loved one receives the highest quality of care in the least restrictive environment. The financial impact is massive—for instance, Texas's 1115 Medicaid waiver has funneled roughly $30 billion to the state over the last decade for uncompensated care and mental health services. You can read more about this specific Texas Medicaid waiver on texastribune.org.
How Waivers Help Your Loved One
Instead of a one-size-fits-all institutional model, waivers fund a broad spectrum of personalized supports. Depending on the specific program, this can include a mix of services like:
- In-home nursing and personal attendant care to help with bathing, dressing, and other daily activities.
- Essential therapies, such as physical, occupational, and speech therapy.
- Respite care to give primary caregivers a much-needed, temporary break.
- Adaptive aids and minor home modifications, like ramps or grab bars, to improve safety.
- Community integration and employment assistance for individuals with disabilities.
Trying to understand the world of Medicaid waiver programs in Texas can feel like trying to learn a whole new language. At The Law Office of Bryan Fagan, we know the emotional weight that comes with these decisions. Our mission is to cut through the confusion and provide clear, compassionate guidance to help you secure the vital services your family needs.
For personalized help with your family's unique situation, schedule a free consultation with our experienced team today.
Finding the Right Fit Among Key Texas Waiver Programs
Choosing the right Medicaid waiver program can feel like trying to find a specific key on a very large, confusing keyring. Each program is designed to unlock a different set of services for a particular group of people. Understanding these differences is the first crucial step in finding the right support for your loved one.
The state of Texas gets it: different life stages and medical conditions require unique approaches to care. A medically fragile child has vastly different needs than an aging adult or an individual with a lifelong developmental disability. This is why Texas offers several distinct waiver programs, each built to provide specific, appropriate support.
Let’s break down the most common options available to Texas families.
Home and Community-Based Services (HCS)
The Home and Community-based Services (HCS) program is one of the most well-known Medicaid waiver programs in Texas. It's specifically designed for individuals with an intellectual or developmental disability (IDD) or a related condition.
The whole point of HCS is to empower individuals to live as independently as possible, whether that’s in their own home or a small, community-based group home. This program offers a broad range of services that go far beyond basic medical care.
Services available through the HCS program often include:
- Residential Support: Assistance in a group home setting or in the individual's own home.
- Day Habilitation: Programs that teach skills for community integration and daily living.
- Employment Assistance: Support in finding and keeping a job.
- Respite Care: Giving primary caregivers a necessary break from their duties.
- Therapies: Access to physical, occupational, and speech therapies.
A common scenario for HCS involves a parent who is also the guardian of their adult child with a significant intellectual disability. The HCS waiver can provide funding for their child to live in a supervised group home, attend a day program, and receive specialized therapies, ensuring they have a full, engaged life within their community.
The CLASS Program
Next up is the Community Living Assistance and Support Services (CLASS) program. While it also helps people live outside of institutions, CLASS focuses on individuals with a "related condition"—a disability, other than an intellectual disability, that started before age 22 and affects their ability to function in daily life.
Many Texas Medicaid waiver programs provide crucial support for individuals with developmental disabilities. The CLASS program specifically helps people with conditions like spina bifida, muscular dystrophy, and Autism (ASD) get the support they need to remain active and independent in their community.
Medically Dependent Children Program (MDCP)
For families caring for a medically fragile child or young adult, the Medically Dependent Children Program (MDCP) is an absolute lifeline. This waiver is designed for individuals under 21 who meet the medical necessity requirements for nursing facility care.
The program's main goal is to prevent institutionalization by providing services that allow these children to get the care they need right in their own family homes. Services under MDCP can include in-home nursing, respite care, and adaptive aids, offering critical support to families facing immense medical and emotional challenges.
STAR+PLUS Home and Community Based Services
The STAR+PLUS waiver program is geared toward adults aged 65 and older, as well as other adults with disabilities. This is often the program families turn to when an aging parent needs help to continue living safely at home instead of moving into a nursing facility.
STAR+PLUS uses a managed care approach, coordinating a whole menu of services to meet an individual's specific needs. This can include personal attendant services, home-delivered meals, emergency response systems, and minor home modifications to improve accessibility.
The breadth of these programs reflects the diverse needs of Texans. As of 2021, state healthcare programs served 418,686 disabled individuals and 2,927,058 children, among others. To get a sense of the sheer scale of these services, you can review key data from the Texas Comptroller's office.
Navigating the various Texas Medicaid waiver programs can be challenging, but understanding the options is the first step. To make it a bit easier, here’s a quick comparison of the key programs we've discussed.
Quick Guide to Key Texas Medicaid Waiver Programs
| Waiver Program Name | Primary Population Served | Common Services Provided |
|---|---|---|
| HCS | Individuals with intellectual or developmental disabilities (IDD) | Residential support, day programs, employment assistance, respite care |
| CLASS | Individuals with "related conditions" (non-IDD) originating before age 22 | Community living support, therapies, adaptive aids, respite care |
| MDCP | Medically fragile children and young adults under 21 | In-home nursing care, respite, adaptive aids, therapies |
| STAR+PLUS | Adults 65+ and other adults with disabilities | Personal care attendants, home modifications, home-delivered meals, respite |
This table provides a high-level overview, but the details of each program can be complex. Choosing the right one depends entirely on your loved one’s unique situation.
Identifying the correct program is a foundational step. Each has its own application process and, unfortunately, its own interest (waiting) list. An experienced attorney can help your family analyze your loved one’s specific needs and identify the waiver that offers the best path forward. For families in Harris County, Montgomery County, or Fort Bend County, understanding these local options is key to effective Estate Planning and long-term care management.
Meeting the Medical and Financial Eligibility Rules
Figuring out if your loved one qualifies for a Texas Medicaid waiver can feel like the most daunting part of this whole journey. The rules often seem complex and unforgiving, but they really boil down to two main hurdles every applicant has to clear: medical eligibility and financial eligibility. Getting a handle on these is the key to building a strong application and steering clear of preventable delays or denials.
At its core, the whole process is about demonstrating need. The state needs to see that your loved one truly requires the level of support these waiver programs offer and that your family's financial picture fits within the specific lines drawn by Medicaid.
Proving Medical Necessity
The first major checkpoint is establishing medical eligibility. For most waiver programs, this means showing that an applicant has a medical need so significant that they would otherwise qualify for care in an institution, like a nursing home. You'll often hear this referred to as meeting the "nursing facility level of care," or LOC.
To determine this, a state-appointed nurse or therapist will conduct a detailed assessment of your loved one's condition and abilities. They'll look closely at their capacity to handle daily activities—things like bathing, dressing, eating, and managing their own medications. The goal is to paint a clear, honest picture of how much they depend on others for care.
This process involves a deep dive into medical records and statements from physicians. As you're gathering and sharing this sensitive information, it's crucial to handle it correctly. Having a good grasp of privacy regulations, like those detailed in this HIPAA compliance requirements checklist, can be a huge help in making sure all personal health information is managed properly. A successful LOC assessment is the first big green light on your path to waiver services.
To help you get a sense of which waiver might be the right fit, this decision tree lays out the different paths based on developmental, medical, or age-related conditions.
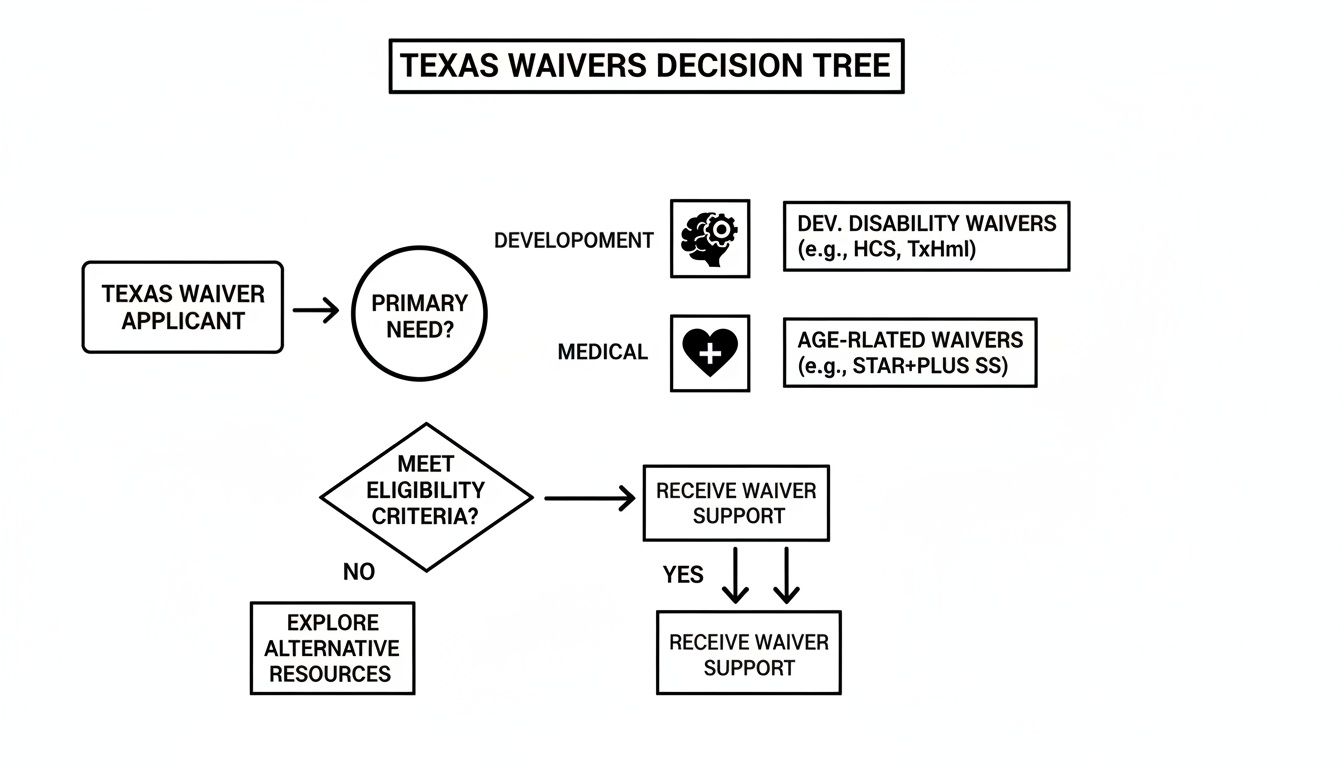
As you can see, the first move is always to identify the primary need, which then points you toward the most appropriate group of waiver programs.
Navigating Strict Financial Limits
Once medical necessity is established, the spotlight shifts to financial eligibility. This is honestly where many families, whether they're in Harris County or Dallas County, start to feel the most stress. Medicaid has incredibly strict limits on both income and the assets that the person applying for benefits can have.
As of 2024, an individual applicant generally can't have more than $2,000 in countable assets.
So, what gets counted?
- Cash in bank accounts (both checking and savings)
- Stocks, bonds, and mutual funds
- A second home or any other property
The good news is that not everything is counted against you. Medicaid typically exempts the applicant's primary home, one car, personal belongings, and any pre-paid funeral plans.
The income rules are just as tough. A person's monthly income has to fall below a specific limit that the state sets each year. But what if your loved one’s income, maybe from a pension or Social Security, is just a little bit over that line? It’s a common and truly heartbreaking problem for countless families.
Using a Miller Trust for Income Eligibility
For those caught in that tough spot—with income too high to qualify but far too low to afford private care—Texas law offers a powerful solution: a Qualified Income Trust (QIT), more commonly known as a Miller Trust.
Think of a Miller Trust as a special legal tool designed specifically to solve this income problem. It works like a funnel. Each month, your loved one's income goes directly into the trust's bank account. From there, the trustee pays for certain medical expenses and a small personal needs allowance, and the rest goes toward their cost of care.
By running the income through the trust, it's no longer counted against the Medicaid income limit. This simple, legal step allows the person to become financially eligible. It’s not a loophole; it’s a legally recognized strategy under both state and federal law designed to help people get the care they desperately need.
Setting up a Miller Trust or exploring other tools like a special needs trust in Texas requires absolute precision to comply with Medicaid's rules. One small mistake in the legal drafting can lead to disqualification. This is where working with an experienced attorney is invaluable. They can ensure these tools are structured correctly, protecting your loved one’s eligibility and giving your family much-needed peace of mind.
Getting on the Interest List and Managing the Wait
The journey to getting Medicaid waiver services in Texas doesn't start with a mountain of paperwork. It begins with a single, crucial step: getting your loved one's name on the interest list. Think of this as the official waiting list, and knowing how to get on it—and how to handle the incredibly long wait—is half the battle. This process is a marathon, not a sprint, and being prepared from day one can make all the difference for your family.
That first step is deceptively simple but absolutely vital. The second you think your loved one might need waiver services down the road is the second you should get their name on a list. For some of the most in-demand programs, the wait can stretch for well over a decade, making early action non-negotiable.
How to Get on the Interest List
Your first practical step is to call the right state agency. For most intellectual and developmental disability (IDD) waivers like HCS and CLASS, you'll need to contact your local IDD authority (LIDDA). For other programs, like MDCP or the STAR+PLUS waiver, you’ll be calling the Texas Health and Human Services Commission (HHSC) or an enrollment broker.
When you make that call, have some basic information ready for the person needing services:
- Their full legal name
- Their date of birth
- Their Social Security Number
- Their current address and contact information
Be direct and clear. A simple "I want to add [Name] to the interest list for the [Program Name, e.g., HCS] waiver program" is all it takes. That phone call officially marks your loved one's place in line.
Managing the Extremely Long Wait
Getting on the list is just the beginning. The wait times for many Medicaid waiver programs in Texas are notoriously long. The HCS interest list, for example, is known to have well over 100,000 names, with families waiting upwards of 15 years. For families in Houston, Dallas, and across the state who need support now, this reality can be emotionally draining.
Waiting for years on end can feel discouraging, but persistence and organization are your best tools. Think of managing the waitlist as an active process, not a passive one. Staying proactive ensures that when your loved one's name finally reaches the top, you are ready to act immediately.
Staying organized is the key to navigating this prolonged period. I always advise clients to create a dedicated folder—either a physical one or a digital one on their computer. In it, you'll keep copies of every letter, notes from every phone call (with the date, time, and who you spoke to), and all other relevant documents. This file will become your single source of truth.
Proactive Steps While You Wait
While you can't jump the line, you absolutely can take steps to ensure you don’t lose your spot. After waiting a decade, losing your place because of a simple mistake would be a devastating setback.
Here are the most important things you need to do:
- Update Your Contact Information: This is the most critical task. If the state can't reach you when your loved one’s name is called, they will simply move on to the next person. Every time you move or change your phone number, you must notify the correct agency in writing.
- Respond to Every Letter: From time to time, the state will send out letters to make sure you're still interested in the services. You have to respond to these letters by their deadline. Missing just one can get you kicked off the list.
- Document Everything: Keep detailed records of your loved one's changing medical needs and conditions. This information will be absolutely essential once you're invited to formally apply and have to go through the medical eligibility assessment.
This long wait is also the perfect time for strategic financial planning. Many families use these years to structure assets to meet the strict Medicaid financial limits, long before an application is ever submitted. Our firm can help you understand your options for protecting assets from nursing home costs and putting your loved one in the best possible position for future eligibility. Managing this wait is a huge emotional and administrative burden, but you don't have to face it alone.
A Guardian's Role in Managing Waiver Benefits

When a court appoints a guardian, that person isn’t just stepping in to help—they are taking on a profound legal and ethical duty to act in the best interest of the individual they protect, known as the ward. This isn't just a suggestion; it's a foundational requirement under the Texas Estates Code, Title 3, Subtitle G. For many, a critical part of upholding this duty involves securing and managing benefits from Medicaid waiver programs in Texas.
The guardian effectively becomes the ward’s chief advocate and decision-maker. This role means dealing with complex state agencies, deciphering detailed program rules, and making tough calls about healthcare and finances. It’s a heavy responsibility that directly shapes the ward's quality of life.
Navigating the Application as a Fiduciary
Let's walk through a common scenario you might see in a Harris County Probate Court. A mother is appointed guardian for her adult son, who has a severe intellectual disability. After years on the HCS interest list, his name is finally called. As his legal guardian, she is now empowered—and expected—to take the lead on the entire application process.
This job involves several key actions:
- Completing and signing all application forms on her son's behalf.
- Gathering and submitting all necessary documents, from medical records to financial statements.
- Communicating directly with HHSC case managers and other state officials.
- Making informed healthcare decisions about the waiver services being offered.
Under the Texas Estates Code, every action the guardian takes must prioritize the ward's well-being. This means meticulously pursuing every available benefit that could enhance the ward's care, independence, and overall happiness.
Managing Finances and Reporting to the Court
A guardian's work doesn't stop once the application is approved. They are also responsible for managing the ward’s finances in a way that keeps them eligible for Medicaid waiver services. This requires a sharp eye on the strict income and asset limits we discussed earlier.
A guardian must make sure the ward’s countable assets stay below the $2,000 threshold. This often means setting up a dedicated bank account for the ward's funds and carefully tracking every dollar spent to avoid accidentally disqualifying them from their benefits.
On top of that, the guardian must account for all of these financial activities to the court. Most Texas courts require guardians to file an Annual Account, which is a detailed report outlining all income received and expenses paid for the ward. This creates a transparent record, proving the guardian is using the ward’s funds—including any waiver benefits—appropriately and for their sole benefit. This is a core part of the ethical management of public benefits a guardian is sworn to uphold.
The Guardian as the Ultimate Advocate
At the end of the day, a guardian is the central point of contact and the lead advocate for the ward within the waiver system. They are the ones attending care planning meetings, coordinating with service providers, and tackling any problems that come up with the quality or delivery of services.
For instance, if a service provider isn't meeting the ward's needs as laid out in their care plan, it is the guardian's legal responsibility to step in. This could mean filing a complaint, finding a new provider, or pushing for changes to the plan. This hands-on management ensures the ward receives the full benefit of the Medicaid waiver programs Texas offers, honoring the court’s trust and the family’s hopes for their loved one.
When to Get Legal Help for Your Family's Journey
Trying to navigate the world of Medicaid waiver programs in Texas on your own can feel like trying to solve a puzzle with half the pieces missing. It’s a genuinely overwhelming process. While many families can handle certain parts, there are critical moments where one wrong move can lead to a denial or a soul-crushing delay.
Knowing when to call in an expert is key to protecting your loved one’s future. An experienced attorney isn’t just an advisor; they become an invaluable partner when the stakes are at their highest. Here at The Law Office of Bryan Fagan, our goal is to bring clarity and a steady hand to these challenging times, preventing costly errors before they ever have a chance to happen.
Critical Moments for Legal Counsel
Some situations are just too complex to handle alone. These aren't just about filling out forms correctly; they require legal strategies that directly impact whether your loved one qualifies and the quality of care they will receive.
It’s time to seek our help when you’re facing scenarios like these:
- Establishing a Guardianship: If your loved one is unable to make their own decisions, you can't simply apply for benefits on their behalf. You'll likely need a court-ordered Guardianship to get the legal authority to act for them.
- Income or Asset Complications: The Medicaid income limit is notoriously strict. When income is even slightly over the cap, a precisely drafted Miller Trust is the only way to secure eligibility without losing benefits.
- Appealing a Denial of Services: Receiving a denial letter is devastating. An attorney can build a strong, evidence-based case for a fair hearing and fight for the benefits your family rightfully deserves.
The legal process is so much more than paperwork. It’s about building a protective legal framework for your loved one. An attorney ensures that every tool, from trusts to guardianships, is implemented correctly to achieve your family’s goals.
Proactive Legal Support Prevents Future Crises
Legal help isn't just for emergencies. In fact, the best time to get support is often before a crisis hits. Think about it this way: after Hurricane Katrina, emergency waivers were created to help vulnerable people in a disaster. The TexKat program, for example, ended up serving nearly 60,000 people, showing just how quickly systems can be forced to adapt. You can discover more insights about these emergency responses from the National Center for Biotechnology Information.
While you might not be facing a natural disaster, a sudden health decline can feel just as urgent. Having a solid legal plan in place means you’re prepared for whatever life throws at you, rather than scrambling when you’re already under immense stress.
The journey through Texas Medicaid waivers is complicated, but you absolutely do not have to walk it alone. The compassionate team at The Law Office of Bryan Fagan is here to answer your questions and provide the personalized support your family needs and deserves.
We understand the emotional and financial weight you are carrying. To talk about your family’s unique situation and create a clear path forward, please schedule a free consultation with us today.
Your Top Questions About Texas Medicaid Waivers Answered
Diving into the world of Medicaid waiver programs in Texas can feel overwhelming, and it almost always stirs up a lot of questions. Let's tackle some of the most common concerns families like yours face, with clear, straightforward answers.
How Long Are the Waiting Lists for Texas Waiver Programs?
This is the million-dollar question, and the answer can be tough to hear. These waiting lists, which the state calls "interest lists," can be incredibly long—often lasting for many years. For popular programs like the HCS and CLASS waivers, it's not uncommon for applicants to wait well over a decade.
The single most important takeaway here is to get your loved one's name on an interest list the moment you even think you might need these services down the road. You can check your spot in line, but unfortunately, there’s no way to jump the queue unless you meet very specific, state-defined crisis criteria.
Can My Loved One Have Assets and Still Qualify?
Yes, but the financial rules are extremely strict. Generally, an individual applying for a waiver can only have about $2,000 in what are called "countable" assets. The good news is that not everything counts. Your primary home, one vehicle, and personal belongings are typically exempt from this calculation.
Things get a bit more flexible for married couples. Special rules, known as spousal protection rules, are in place to allow the healthy spouse to retain a larger portion of the couple's assets. Navigating this is tricky, which is where an attorney can step in. They can use legal tools like a Special Needs Trust to protect assets while ensuring your loved one remains eligible for the care they need.
What Should We Do If Our Application Is Denied?
Receiving a denial notice is disheartening, but it's not the end of the road. You have the right to appeal the decision. The notice you receive will spell out why the application was denied and give you a deadline for filing an appeal, which triggers a process called a fair hearing. This hearing is your opportunity to present your side of the story and provide evidence showing that your loved one does, in fact, meet the program's criteria.
This is one of those times when having legal representation can make all the difference. An experienced attorney knows how to build a strong case, gather the right medical and financial evidence, and argue on your behalf in front of the hearings officer. It gives you the best possible shot at overturning the denial.
Your family’s situation is unique, and you shouldn’t have to navigate this complex system alone. At The Law Office of Bryan Fagan, PLLC, we’re here to provide the clear guidance and compassionate support you need to secure the best care for your loved one. Whether you need help with guardianship, setting up a trust, or appealing a waiver denial, we're ready to help. Schedule your free, no-obligation consultation today by visiting https://texasguardianshiplawyer.net.







